Your Second Brain: The Bizarre and Crucial Connection Between Your Gut and Your Mental Health
Gut Brain Connection Mental Health reveals how your gut influences mood, memory, and more in surprising ways you need to know today.
Have you ever found something weird in a game that totally wasn’t supposed to be there? Back in the original Pokémon Red and Blue, a glitch called MissingNo. did just that. When you fished on Cinnabar Island, a strange blocky glitch would appear, looking like static and causing crazy effects. It could mess up your game, corrupt your Hall of Fame, and make your graphics go wild.
But here’s the crazy part: players actually loved MissingNo.! Catching it meant you could duplicate items like Rare Candies or Master Balls, basically giving you unlimited powerful items. What started as a glitch turned into a fan-favorite secret cheat. It’s wild how a programming bug became such a legend in gaming history.
Ever wondered why your mood sometimes feels tied to your stomach? The Gut Brain Connection Mental Health is more than just a mystery—it’s a fascinating biological conversation happening inside you right now. Dive in to explore how your gut might be the surprising key to understanding your mental well-being.
Understanding the gut brain connection: basics and significance
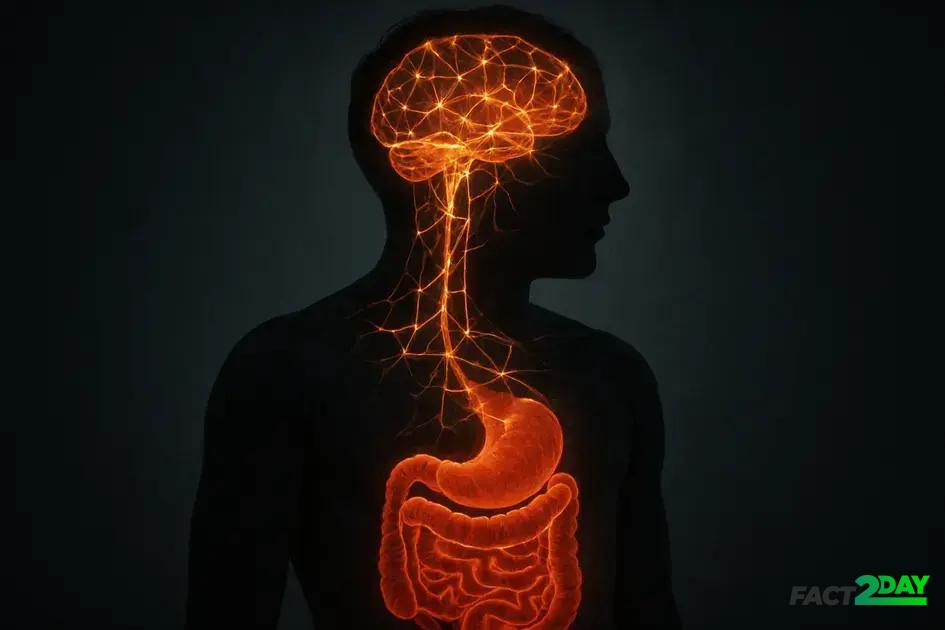
The gut brain connection refers to the complex communication network between your gastrointestinal system and your brain. This connection is crucial because it helps regulate digestion, mood, and overall mental health. Millions of neurons line your gut, sometimes called the “second brain,” allowing it to operate independently and send signals to the brain.
This communication happens through multiple pathways, including the nervous system, immune responses, and biochemical signals. One key player is the vagus nerve, which acts like a highway sending messages back and forth between the gut and brain. These signals help the brain understand what’s going on in your digestive tract, influencing feelings, cravings, and even behavior.
Understanding these basics is important because disruptions in this communication can contribute to mood disorders like anxiety or depression. It also sheds light on why gut health extends far beyond digestion and impacts mental well-being. Maintaining a healthy gut can be a powerful way to support your brain and emotional health.
How the gut microbiome influences your mental health
The gut microbiome is a community of trillions of bacteria, viruses, and fungi living in your digestive tract. These tiny organisms play a vital role in not only digestion but also your mental health. Research shows that the balance of these microbes can influence your mood, stress levels, and even cognitive function.
Microbial Balance and Brain Chemistry
Gut bacteria produce chemicals like serotonin, dopamine, and gamma-aminobutyric acid (GABA), which act as neurotransmitters affecting the brain. In fact, about 90% of the body’s serotonin is made in the gut. When the microbiome is healthy, it supports proper production and balance of these mood-regulating chemicals.
Impact of Dysbiosis
An imbalance in gut microbes, called dysbiosis, can lead to increased inflammation and disrupt the gut-brain axis. This may contribute to anxiety, depression, and other mood disorders. Studies have linked gut dysbiosis with conditions such as irritable bowel syndrome (IBS), which often coexists with mental health challenges.
Supporting Mental Health Through the Microbiome
Maintaining a diverse and balanced microbiome is key. Eating fiber-rich foods, fermented products like yogurt and kimchi, and reducing processed foods can help nurture beneficial bacteria. Probiotics and prebiotics are also being researched for their potential to improve mental well-being by restoring healthy gut flora.
The role of neurotransmitters produced in the gut
The gut produces many key neurotransmitters that affect how we feel and think. These chemical messengers help transmit signals between nerve cells and play a major role in mood regulation, stress response, and cognitive functions.
Serotonin: The Mood Stabilizer
About 90% of the body’s serotonin, often called the “feel-good” neurotransmitter, is produced in the gut. It regulates mood, appetite, and sleep. A balanced gut ensures healthy serotonin production, which is crucial for emotional well-being.
Dopamine: The Reward Chemical
Dopamine influences pleasure, motivation, and focus. Gut bacteria help synthesize dopamine precursors, supporting the brain’s ability to regulate behavior and reward mechanisms.
Gamma-Aminobutyric Acid (GABA)
GABA is an inhibitory neurotransmitter that calms nervous system activity. Certain gut microbes produce GABA, which can help reduce anxiety and promote relaxation.
The complex interactions between these neurotransmitters and the brain highlight the gut’s powerful role in shaping mental health. Supporting gut health can boost neurotransmitter balance and improve overall emotional stability.
Impact of gut inflammation on mood disorders
Gut inflammation happens when the immune system reacts to harmful bacteria or irritants in the digestive tract. This inflammation can disrupt the gut’s normal function and harm the balance of beneficial microbes. Research shows a strong link between gut inflammation and mood disorders like depression and anxiety.
The inflammation and brain connection
When the gut is inflamed, it releases chemicals called cytokines. These pro-inflammatory cytokines can travel through the bloodstream and affect the brain, leading to changes in mood and behavior. This process is often called the gut-brain inflammation axis.
How inflammation affects mood disorders
Chronic inflammation in the gut may interfere with neurotransmitter production and brain function. It can reduce serotonin levels and increase stress hormones, making people more prone to feeling anxious or depressed. Many people with mood disorders show signs of increased gut inflammation.
Reducing gut inflammation for better mental health
Improving gut health by eating anti-inflammatory foods like fruits, vegetables, and omega-3 fatty acids can support mood. Avoiding processed foods and chronic stress also helps prevent inflammation. In some cases, doctors recommend probiotics or medications to target inflammation directly.
Understanding the role of gut inflammation opens new doors to treat mood disorders by focusing on the gut-brain connection.
The vagus nerve: your body’s communication highway
The vagus nerve is a key part of the nervous system connecting your brain to many organs, including the gut. It acts like a communication highway, sending messages between the brain and the digestive system to help control digestion, heart rate, and even mood.
How the vagus nerve works
The vagus nerve sends signals both ways – from the gut to the brain and back. This two-way communication is vital for maintaining balance in the body. For example, when you eat, the vagus nerve tells your brain about the state of digestion and can also trigger feelings of fullness.
Vagus nerve and mental health
Stimulating the vagus nerve has been linked to reduced anxiety and depression. It helps the brain regulate stress responses and releases neurotransmitters that calm the nervous system. Techniques like deep breathing, meditation, and cold exposure can boost vagus nerve activity.
Impact on gut health
The vagus nerve also helps control inflammation in the gut by signaling the immune system. Proper vagus nerve function supports a healthy gut environment, which in turn benefits mental well-being.
Understanding the vagus nerve shows how closely connected your mind and body truly are.
Can diet improve mental health by targeting the gut?
Your diet plays a critical role in shaping your gut health, which in turn affects mental well-being. The foods you eat influence the diversity and balance of gut bacteria, impacting mood, cognition, and stress levels.
Foods that promote a healthy gut and mind
Eating fiber-rich fruits, vegetables, and whole grains supports beneficial bacteria that produce important compounds like short-chain fatty acids. Fermented foods such as yogurt, kefir, and sauerkraut provide probiotics that can boost gut health and potentially ease anxiety and depression symptoms.
Foods to approach with caution
Diets high in processed foods, sugar, and unhealthy fats may disrupt gut balance and promote inflammation. This disruption can negatively affect brain function and mood. Limiting these foods while focusing on nutrient-dense options is important.
The role of omega-3 fatty acids and antioxidants
Omega-3s found in fish and nuts have anti-inflammatory effects that benefit the gut and brain. Antioxidant-rich foods help reduce oxidative stress, supporting overall mental health.
By choosing a diet that nurtures your gut microbiome, you create a strong foundation for better mental health.
Probiotics and prebiotics: mental health allies or myths?
Probiotics and prebiotics are often discussed as helpful agents for gut health, but their impact on mental health is still being studied. Probiotics are live beneficial bacteria found in some foods and supplements, while prebiotics are fibers that feed these bacteria.
How probiotics might support mental health
Some studies suggest that probiotics can improve symptoms of anxiety and depression by restoring balance to the gut microbiome. They may influence mood by producing neurotransmitters and reducing inflammation in the gut.
The role of prebiotics
Prebiotics help grow and maintain healthy bacteria in the gut. A diet rich in prebiotic fibers, found in foods like garlic, onions, and bananas, supports the microbiome, which might indirectly benefit mental health.
What the research says
Research is promising but not yet conclusive. While some clinical trials show mental health improvements with probiotics and prebiotics, others find minimal effects. Variations in strains, dosages, and individual differences make it complex.
Overall, probiotics and prebiotics can be part of a healthy diet, but they are not standalone cures for mental health conditions. More research is needed to fully understand their benefits.
Stress, gut health, and their combined effect on the brain
Stress can directly impact gut health by disrupting the balance of gut bacteria and increasing inflammation. When you experience stress, your body releases hormones like cortisol that influence both the brain and the digestive system.
How stress affects the gut
Under stress, the gut may become more permeable, a condition often called “leaky gut,” which allows harmful substances to enter the bloodstream. This can trigger inflammation and further disrupt the gut microbiome.
The gut’s impact on the brain
A disrupted gut sends distress signals to the brain through the nervous system and immune system, potentially worsening mood disorders like anxiety and depression. The gut and brain influence each other closely via the gut-brain axis, creating a feedback loop.
Managing stress for gut and brain health
Practices such as mindfulness, exercise, and a healthy diet rich in fiber and probiotics can help reduce stress and support gut health. Taking care of both stress and gut function is important for maintaining a balanced mind and body.
Understanding the connection between stress, gut health, and brain function helps explain why emotional well-being is deeply linked to what happens in your digestive system.
The effects of antibiotics and medications on gut brain balance
Antibiotics and other medications can have a significant impact on the delicate balance between the gut and brain. While antibiotics are essential for fighting bacterial infections, they can also disrupt the gut microbiome by killing both harmful and beneficial bacteria.
How antibiotics affect the gut-brain axis
When antibiotics reduce the diversity of gut bacteria, they may impair the production of neurotransmitters and weaken immune responses. This imbalance can lead to digestive issues and changes in mood or cognition.
Medications beyond antibiotics
Other common drugs like antidepressants, antacids, and non-steroidal anti-inflammatory drugs (NSAIDs) can also affect gut health. Some may alter gut motility, change microbiome composition, or increase inflammation, indirectly influencing brain health.
Protecting the gut-brain balance while using medications
To minimize negative effects, it’s important to use antibiotics responsibly and follow medical advice. Supporting gut health with probiotics, prebiotics, and a balanced diet can help restore microbiome diversity during and after treatment.
Understanding how medications impact the gut brain balance underscores the need for careful management to support mental and digestive health.
Gut brain connection in depression and anxiety disorders
The gut brain connection plays a significant role in depression and anxiety disorders. Changes in the gut microbiome can affect how the brain regulates mood, stress, and emotions, sometimes worsening symptoms of these disorders.
How gut health impacts depression and anxiety
Imbalances in gut bacteria can increase inflammation and alter neurotransmitter levels, such as serotonin and GABA, which are crucial for mood stability. This disruption may lead to feelings of sadness, worry, and stress.
Research findings
Studies have found that many people with depression or anxiety have different gut microbiomes compared to healthy individuals. These differences suggest a strong link between gut health and mental health disorders.
Potential treatments targeting the gut
Emerging treatments like probiotics, prebiotics, and dietary changes aim to restore gut balance to improve mental health. While promising, more research is needed to understand how effective these approaches are for depression and anxiety.
Recognizing the gut brain connection in these disorders highlights the importance of a holistic approach to mental health care.
Emerging research: fecal transplants and mental health
Fecal transplants, also known as fecal microbiota transplantation (FMT), involve transferring stool from a healthy donor to the gut of a patient. This procedure aims to restore a balanced gut microbiome and has been used successfully to treat some digestive diseases.
Fecal transplants and mental health
Emerging research suggests that FMT might impact mental health by improving the gut brain connection. Studies in animals and limited human trials show potential benefits for conditions like depression and anxiety, though the research is still in early stages.
How FMT may work
By introducing diverse, healthy bacteria, FMT can reduce inflammation and help restore neurotransmitter production. This in turn may influence mood and cognitive function through the gut brain axis.
Challenges and future directions
While promising, FMT is not yet widely accepted for mental health treatment. More studies are needed to understand its safety, effectiveness, and long term impact. Researchers are also exploring ways to develop targeted microbiome therapies based on FMT principles.
FMT research highlights a fascinating new frontier where gut health and mental wellness intersect, offering potential for innovative therapies.
Lifestyle habits that support a healthy gut brain axis
Maintaining a healthy gut brain axis requires adopting lifestyle habits that support both gut and mental health. These habits help preserve the balance of gut bacteria, reduce inflammation, and promote clear communication between the gut and brain.
Balanced diet and hydration
Eating a variety of fruits, vegetables, whole grains, and fermented foods provides essential nutrients and prebiotics to feed beneficial gut bacteria. Staying hydrated helps digestion and nutrient absorption.
Regular physical activity
Exercise has been shown to improve gut microbiome diversity and reduce stress hormones. It also supports brain function and mood by promoting the release of endorphins and reducing inflammation.
Stress management techniques
Practices like meditation, deep breathing, and adequate sleep can enhance vagus nerve function, helping maintain gut-brain communication and lowering stress-induced gut issues.
Avoiding harmful substances
Limiting alcohol and avoiding smoking preserves gut lining health and microbiome balance. These substances can disrupt the gut-brain axis and increase inflammation.
By integrating these lifestyle habits, you create a strong foundation for a balanced gut brain axis and improved overall well-being.
Future directions in gut brain connection therapies
Future therapies targeting the gut brain connection are rapidly evolving, offering new ways to treat mental health and digestive disorders. Researchers are exploring innovative methods to restore gut microbiome balance and improve communication between the gut and brain.
Personalized microbiome treatments
Advancements in microbiome analysis allow for tailored treatments that consider an individual’s unique gut bacteria to optimize mental and gut health outcomes.
Next-generation probiotics and prebiotics
Scientists are developing more effective probiotics and prebiotics designed to specifically enhance beneficial gut bacteria involved in mental health regulation.
Microbiome editing and synthetic biology
Emerging tools like CRISPR may enable precise modification of gut bacteria, potentially correcting imbalances linked to mood disorders and cognitive issues.
Gut-brain axis neuromodulation
Technologies stimulating the vagus nerve and other neural pathways aim to improve gut-brain signaling, offering new avenues for treating depression, anxiety, and other conditions.
These exciting developments highlight a future where gut brain connection therapies become key components in holistic health care.
Understanding the Gut Brain Connection is Key
The gut brain connection plays an important role in both mental and physical health. By learning how the gut and brain communicate, we can better support our well-being through lifestyle choices and emerging treatments.
Simple habits like eating a balanced diet, managing stress, and exercising can have a big impact on this powerful connection. New research and therapies are opening exciting paths to improve mental health by targeting the gut.
Keeping the gut and brain in balance offers hope for better mood, cognition, and overall quality of life.




